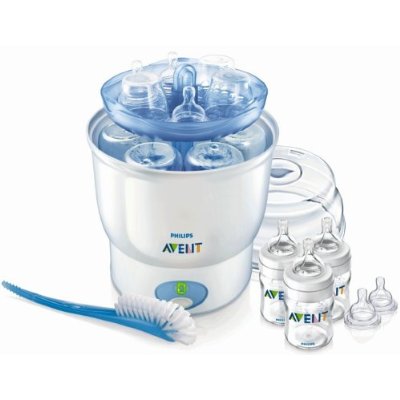
Sterilizator electric de biberoane Philips Avent Advanced SCF291/00, tava de scurgere, sterilizare in 10 min, design compact, 220V - eMAG.ro

Sterilizator electric si uscator de biberoane Philips Avent Premium SCF293/00, Sterilizare si uscare in 40 de min, Tava de scurgere, Design compact, 220V (Alb) - evoMAG.ro