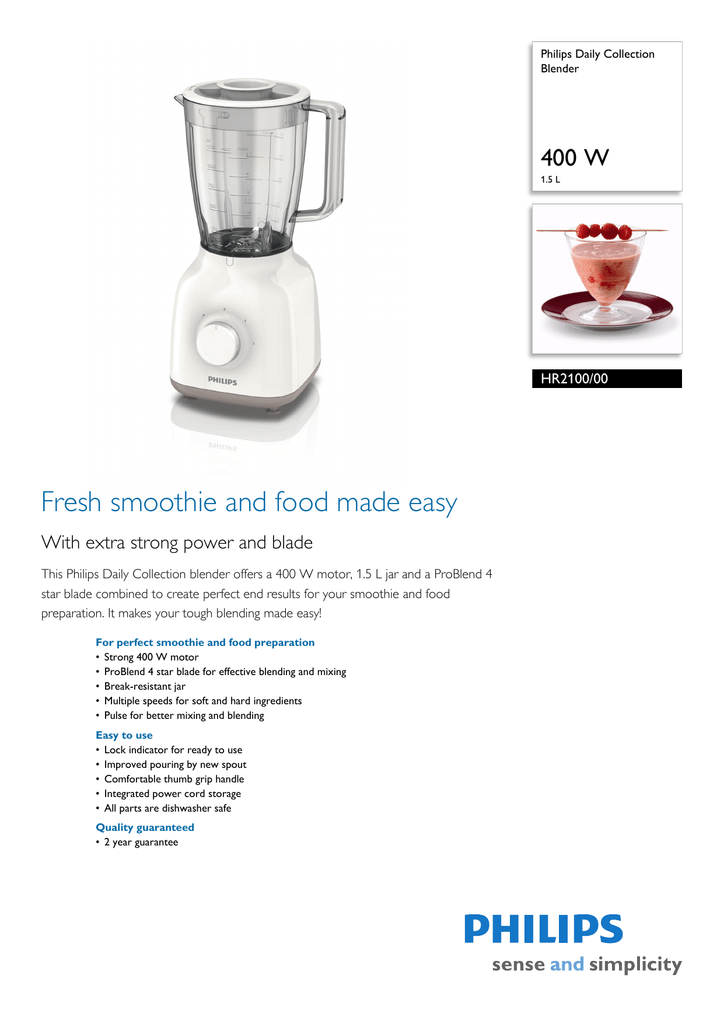
EAN 8710103700623 - Philips Daily Collection Blender Hr2100 400 W 1.5 L Plastic Jar 2 Speed And Puls | upcitemdb.com
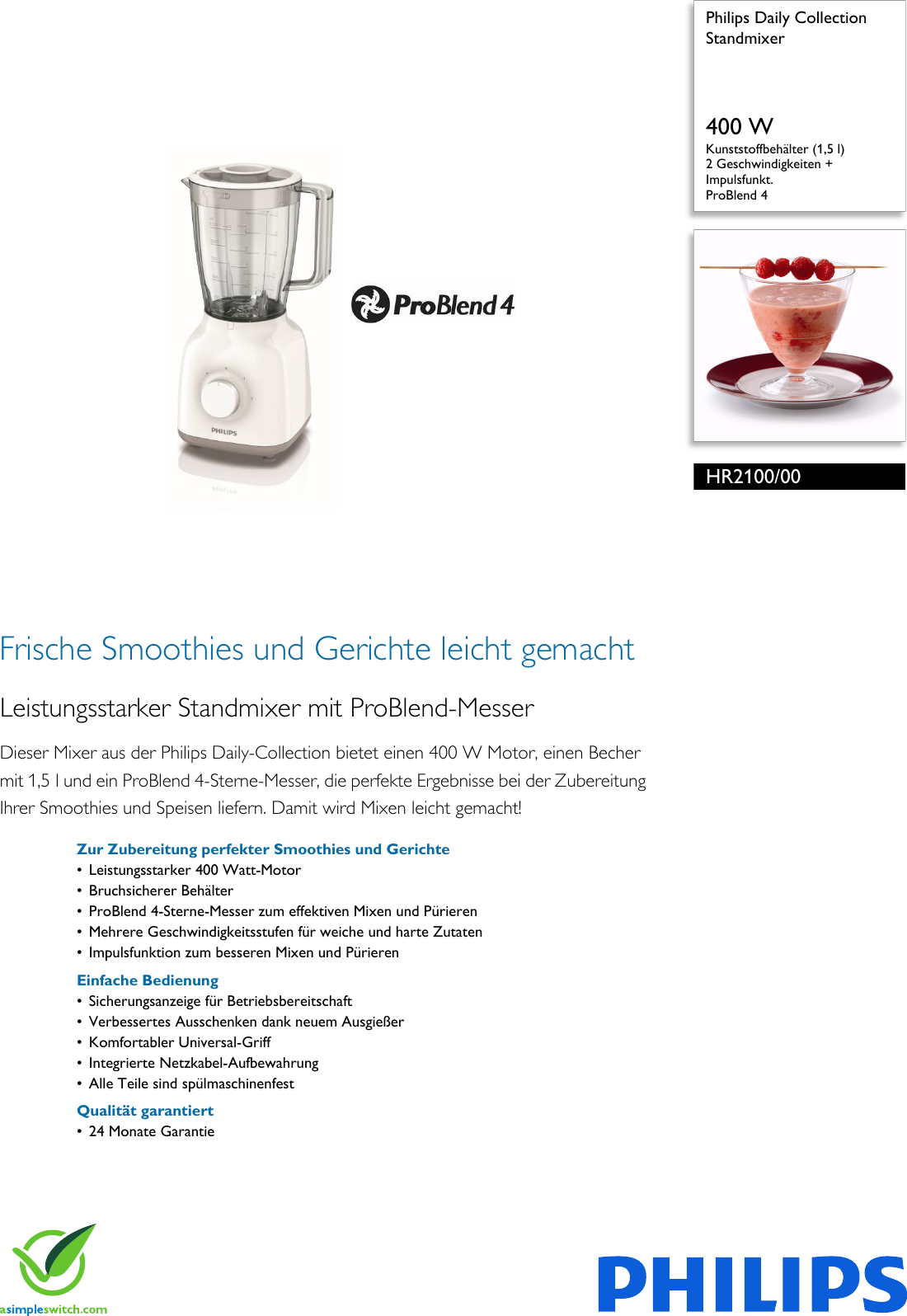
Philips HR2100/00 Leaflet HR2100_00 Released Germany (German) User Manual Datenblatt Hr2100 00 Pss Deude

Philips Blender Daily Collection HR2100/00 Tabletop, 400 W, Jar material Plastic, Jar capacity 1.5 L,

Amazon.com: Plastic Jar For Philips Daily Collection Blender HR2100 HR2102 HR2103 HR2104 HR2108 HR2109 HR2113 HR2114 HR2119 HR2123 HR2124 HR2140 HR2145 HR2146 HR2150 HR2901 HR2904 HR2905 HR3448 996510056884: Home & Kitchen

PHILIPS / Stationary blender HR2100 / 00, 400 W, 2 speeds, bowl 1.5 L, plastic, white (93105) buy at Global Rus Trade

Philips Blender Daily Collection HR2100/00 Tabletop, 400 W, Jar material Plastic, Jar capacity 1.5 L,