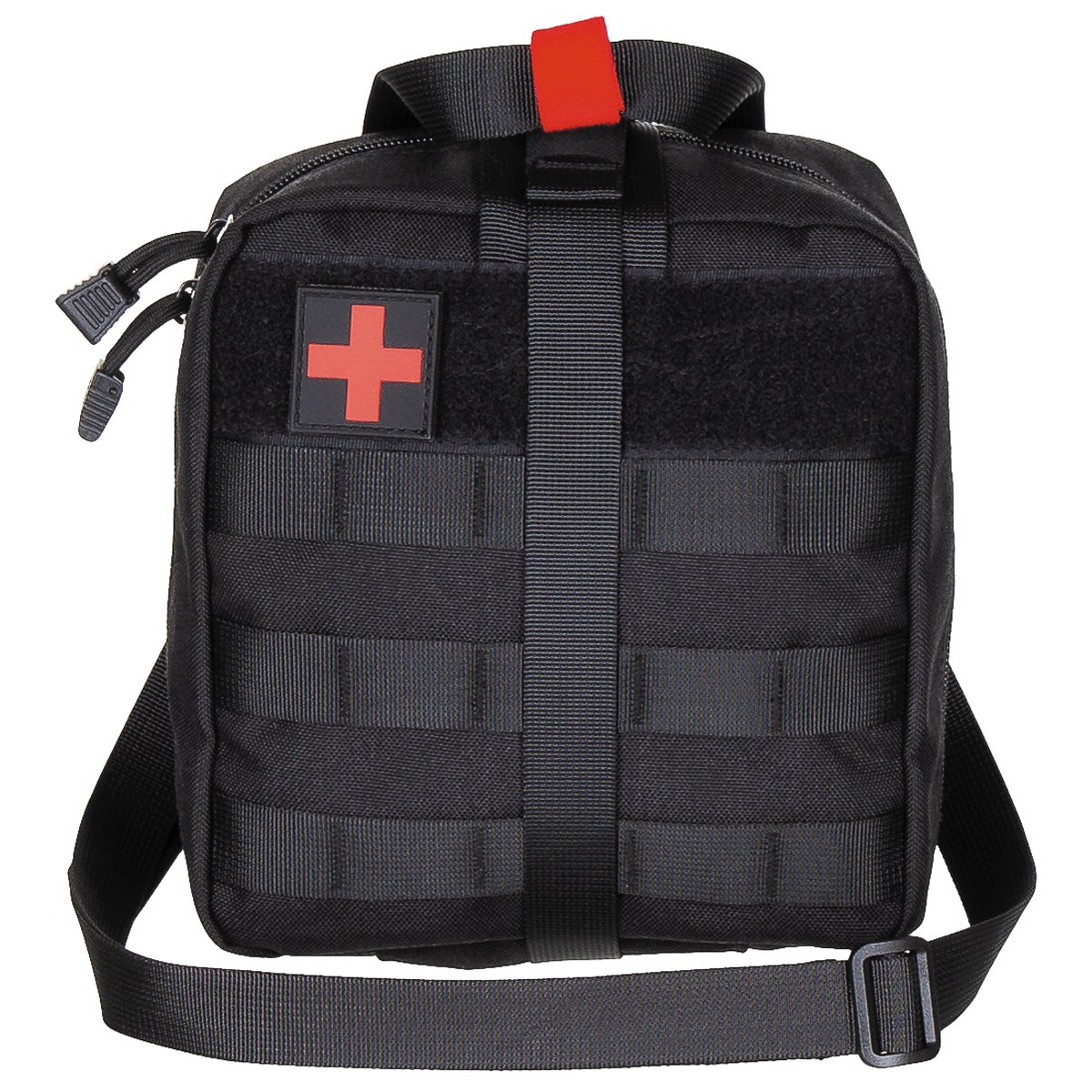
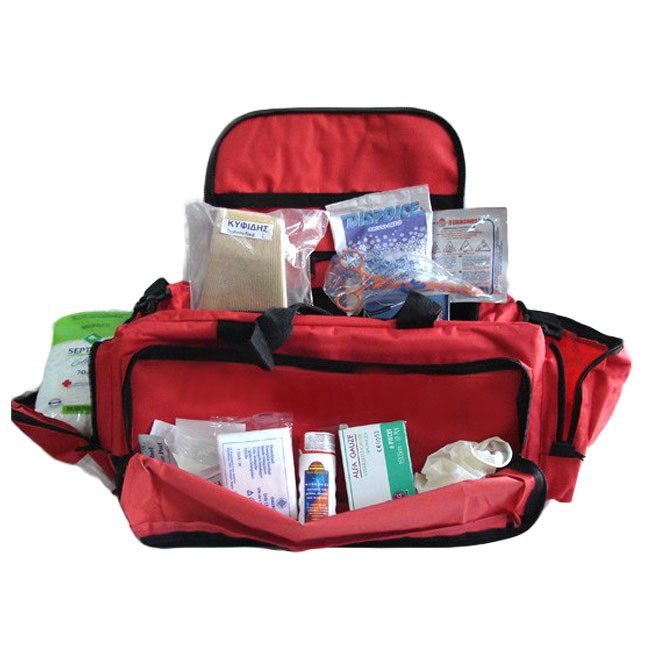
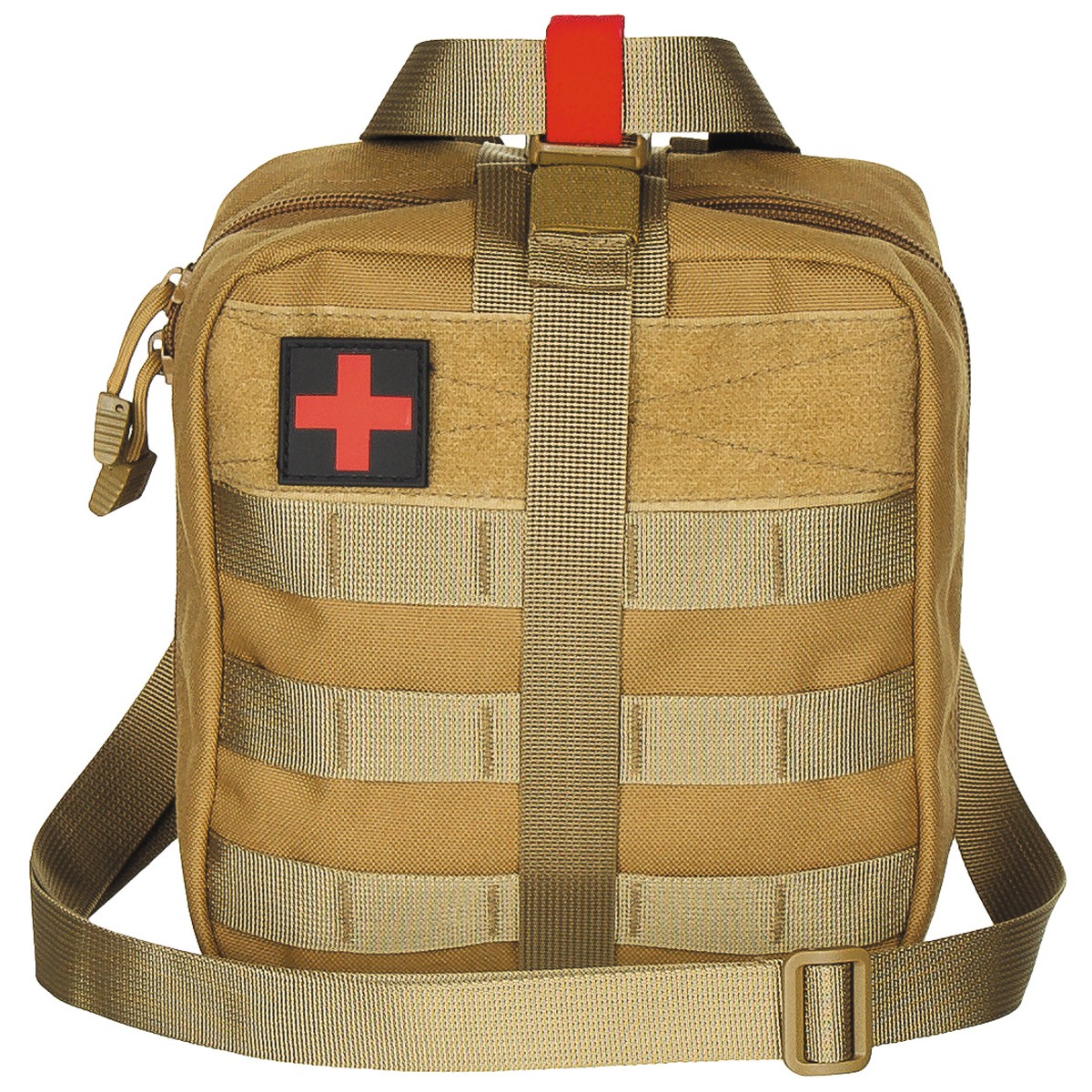
Vojaško Taktično Molle Torbica Za Prvo Pomoč Kompleti Medicinske Vrečko Najlon Zunanji Lov Avto Sili Kampiranje Vojske Preživetje Orodje Eos Vrečko - popust > www.chlorys.si

Torba za prvo pomoč - Torbe in nahrbtniki - Prva pomoč - Lingas Gasilska vozila Bremach, zaščitna in reševalna oprema

Kitajska torba za prvo pomoč z dobavitelji in proizvajalci ročaja - Prilagodite torbo za prvo pomoč z roko na debelo - Gauke
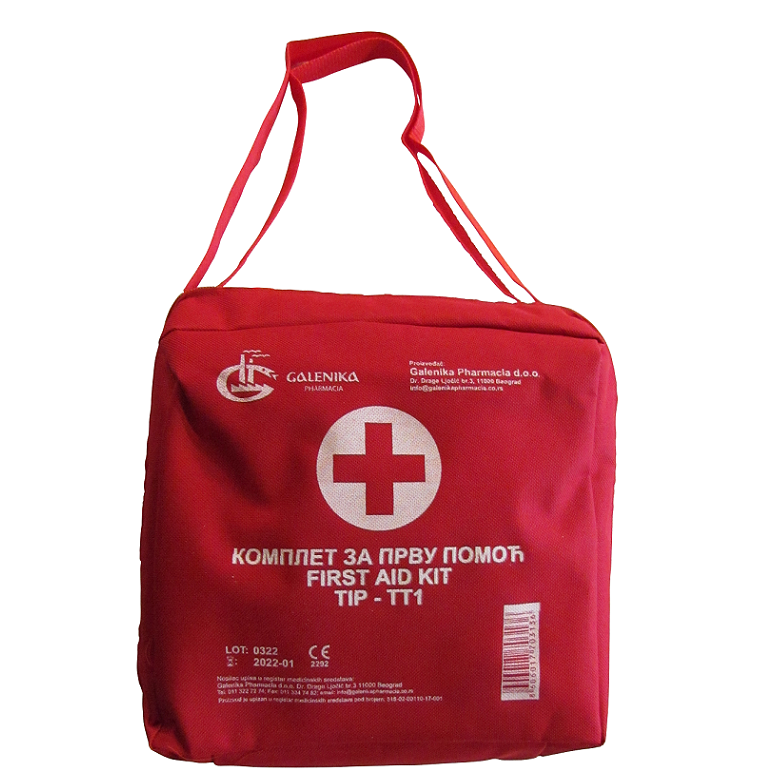
Albo - HBRM - First aid and pharmacies - PORTABLE MEDICAL BAG – FIRST AID KIT TT1, FILLED - Zaštitna i radna odeća, obuća, lična zaštitna oprema...

Prazna torbica za prvo pomoč Lifesystems - Kibuba, pustolovščina na obzorju: Spletna trgovina z gorniško opremo

Torbica za prvo pomoč Waterproof - Kibuba, pustolovščina na obzorju: Spletna trgovina z gorniško opremo

Torbica za prvo pomoč Lifesystems Trek - Kibuba, pustolovščina na obzorju: Spletna trgovina z gorniško opremo

Pripomoček Za Prvo Pomoč IFAK Vrečko Le Molle Nujne Medicinske Bil Reševalec Torbica Vojaške Prostem Reševalne Paket Potovanja Lov Rdeče Črno Ta Kategorija športne Torbe