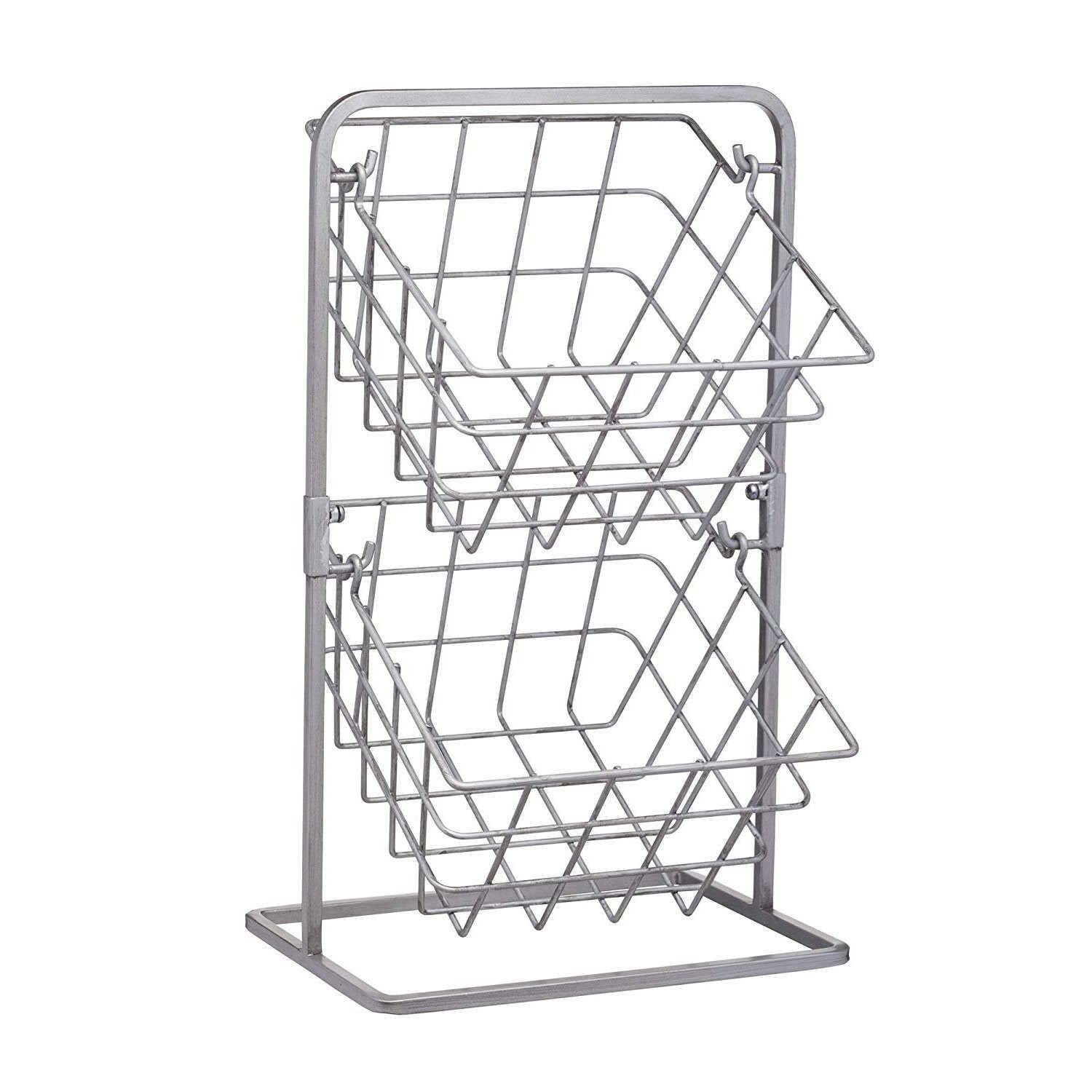
Coș pentru legume și fructe suspendat pe perete Coș cu fructe împletit din răchită naturală Masă de bucătărie Coș de depozitare suspendat pe perete Raft uscat - Baduglobal.ro

Vanzare Frigider Cutie De Depozitare Organizator Frigider Legume Proaspete Fructe Cutii De Golire Coș De Depozitare Containere Cămară, Bucătărie Organizator ~ Casa De Depozitare & Organizare / www.andreimuresanusud.ro

Bucătărie depozitare coș multi-funcțional legume fructe, rafturi cu capac sertar pentru organizatori cutie durabil cumpara - Bucătărie Depozitare & Organizare / www.viewnews.ro

Poze : lemn, alimente, legume şi fructe, maro, mobila, coş, de răchită, depozitare, coșuri, produs natural, zambilă de apă, omul a făcut obiectul, familie iarbă 5852x3675 - - 1192199 - Poze frumoase - PxHere