
Canapea Expomob KING extensibila, 3 locuri, cu arcuri si lada depozitare, dimensiune 180x87x88 cm, culoare gri
CANAPEA EXTENSIBILA, PETIT BEAUTE 180CM, COD 40835, CULOARE GALBEN/MUSTAR, DESIGN MODERN - Artim Group

Cauti Canapea extensibila galbe/gri Zalina 147 cm tapiterie textila, picioare lemn, SPIKEIISZ - Signal?Alege din mii de produse premium de la Mobilado

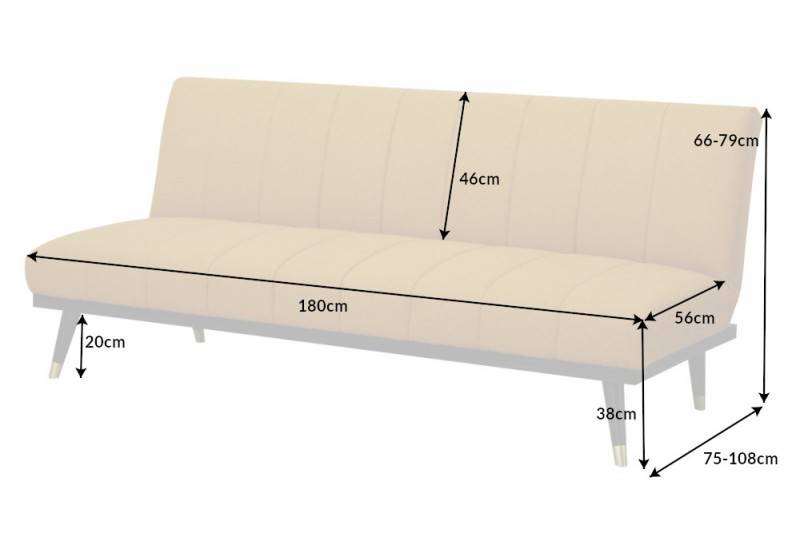
Canapea extensibila galben mustar din poliester si lemn 180 cm Petit Beaute The Home Collection | The Home.ro

Canapea extensibila AIX©, material stofa, 3 locuri, dimensiuni L 180 x l 90 x H 80 cm, culoare albastru - eMAG.ro



















