[ad_1]
The COVID-19 pandemic has been a long and rocky road, and two words have come to symbolize its exit ramp: herd immunity.
Since the start of the vaccine rollout, public officials have stressed that immunizing enough of the population would eventually stop the spread of the coronavirus. Each day, an online dashboard tracks San Diego County’s progress toward that goal.
But what happens once we reach it?
If you’re expecting the virus to vanish, think again, says Natasha Martin, an infectious disease modeler at UC San Diego.
“The biggest misconception is that something magical and immediate and drastic will happen when we hit this level of immunity,” she said.
“It will come with a whimper, not a bang.”
That’s in part because we’re already seeing the benefits of vaccination. Immunizing close to the entire population against COVID-19 would help further, protecting both the vaccinated and unvaccinated. But getting to that point will be a struggle due to the rise of viral variants and issues of vaccine hesitancy and access. And we’re already seeing a clear slowdown in the pace of the rollout.
Martin and many others — including Dr. Anthony Fauci, the nation’s top infectious disease expert — say it’s even possible that we’ll never quite reach herd immunity. But they also say that continuing to vaccinate as many people as possible, as quickly as possible will allow us to live alongside the virus safely by making infections less frequent and less severe.
In other words, the pandemic will end, but expect the coronavirus to stick around.
The safety of the herd
Vaccines protect communities by depriving a virus of the one thing it can’t do without: hosts.
Viruses are essentially teeny-tiny parasites. They slip inside your cells, take them hostage and create countless viral copies that spew out of infected cells, often killing them in the process. And then they repeat that process again and again.
If enough people have been vaccinated or recovered from infection, that leaves fewer places for a virus to go, eventually breaking the cycle of transmission. And that point is known as herd immunity.
Herd immunity doesn’t just help the vaccinated; it helps those who haven’t gotten their shots, or who’ve been inoculated but didn’t mount a strong immune response. That’s because these people, who are still vulnerable to COVID-19, are now mostly in contact with immune individuals, who are far less likely to spread the virus.
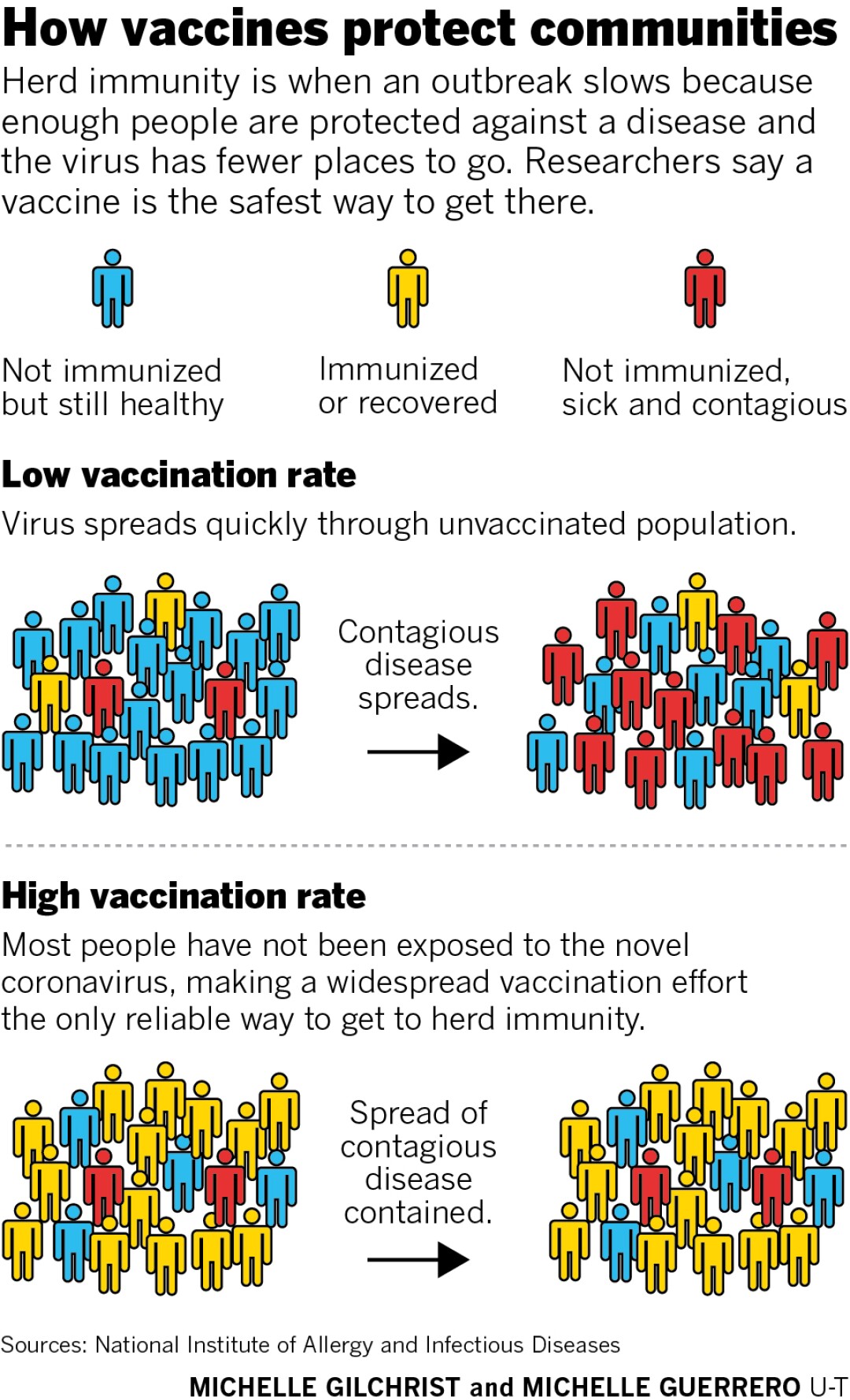
“That person who is in the herd but didn’t perhaps get the vaccine or get the full protection from the vaccine, they’re also protected because the herd is protected,” said Dr. Davey Smith, UCSD’s chief of infectious disease research.
These aren’t hypothetical, far-off benefits of vaccination. They’re already happening and have helped get us to a point where, on Monday, the county reported just 47 new cases, the lowest count since April 2020.
“I do believe that the reductions in case rates that we’ve seen recently are occurring predominantly because of the expansion of vaccinations,” Martin said.
But she cautions that we still haven’t immunized enough people to avoid a potential resurgence in cases if everyone (especially the unvaccinated) suddenly abandoned basic public health precautions.
Reaching herd immunity could prevent surges in a mask-free future. But how many people need to be vaccinated to get there? Martin’s best estimates are in the range of 85 percent to 90 percent, perhaps more.
Those figures apply to the entire population, meaning about 3 million people in San Diego County would need to be vaccinated or have recovered from COVID-19. That’s far higher than the county’s goal of fully vaccinating 75 percent of San Diegans 12 and up, roughly 2.1 million people.
Martin thinks a higher target is warranted for a few reasons. One is that while children younger than 12 aren’t yet eligible for coronavirus vaccines, they, too, can get COVID-19. Another factor is the rise of faster-spreading viral variants, especially B.1.1.7, a strain first spotted in the U.K. and that now accounts for most new cases in the U.S. There’s evidence that this variant is 40 percent to 50 percent transmissible.
It’s going to take time to reach those high levels of community-wide immunity, especially since the pace of vaccination has slowed. The number of San Diegans getting their first vaccine dose has declined for six weeks in a row, from about 123,500 a week in early April to nearly 60,000.
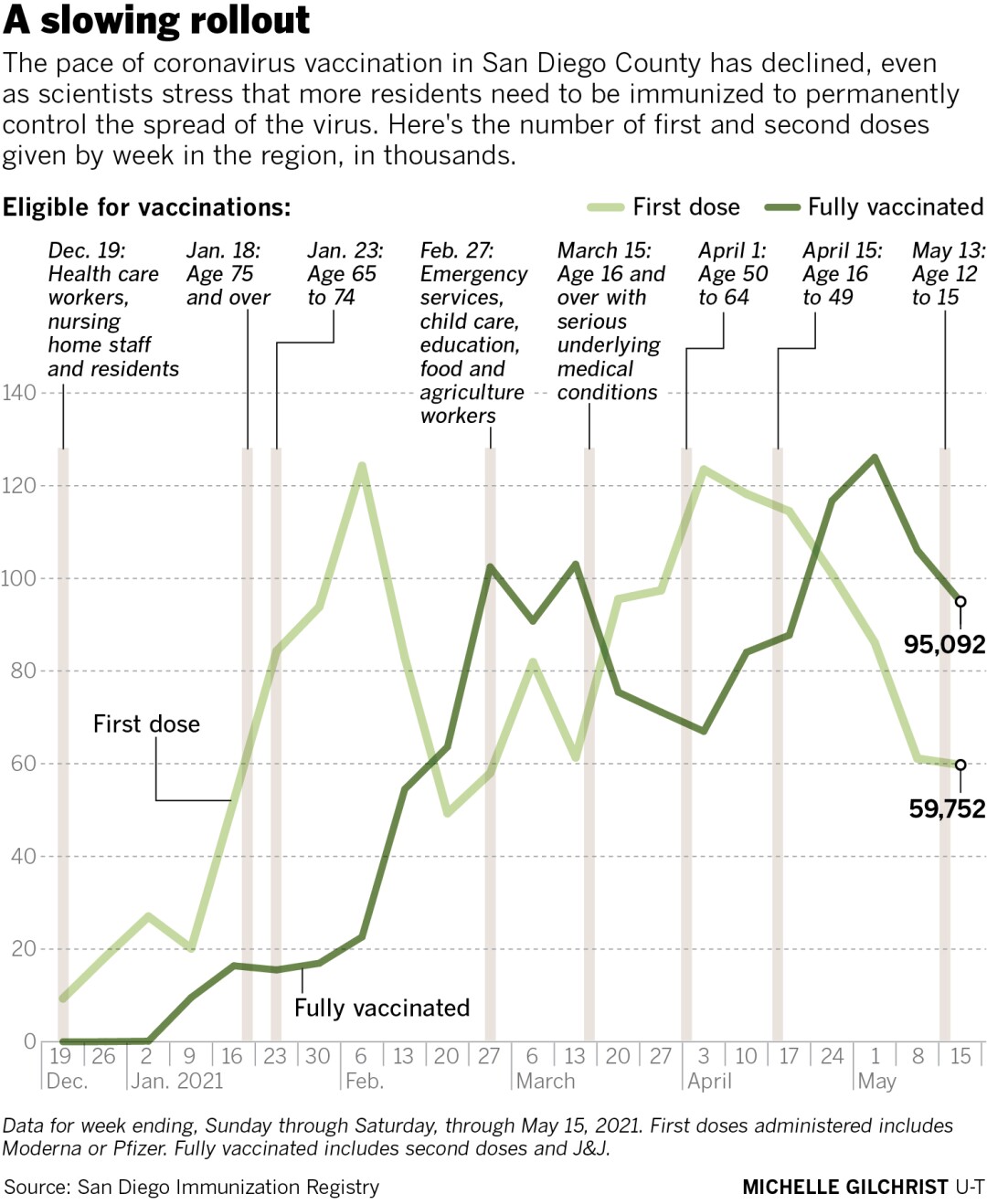
So far, 1.4 million residents have gotten the single-shot Johnson & Johnson vaccine or the two shots of the Moderna and Pfizer vaccines needed for full immunity against the coronavirus. At the current rate, it’s unlikely the county will reach 2.1 million fully vaccinated San Diegans by their goal of early July, let alone the higher figures Martin believes are needed.
“We know it’s going to be a little bit of a grind,” said Supervisor Nathan Fletcher during the county’s weekly coronavirus briefing on Thursday. “We’re going to continue to strive to hit that goal. I think we will at some point get there. It is more an organizing tool around giving us something to strive toward.”
No magic moment

Jaeden Johannesson, Ashley Skoglund and Emily Skoglund, from Minnesota, take a selfie near some sea lions in La Jolla on Tuesday, April 27, 2021 after the CDC said that fully vaccinated people can go outdoors without masks, except in crowded settings.
(Sandy Huffaker / For The San Diego Union-Tribune)
Regardless of when we cross that goalpost, infection rates likely won’t dip dramatically. As people start getting together more, the virus will have more chances to find those who haven’t been vaccinated. And slow but steady vaccination offset by people resuming pre-pandemic activities will probably mean case rates will continue declining gradually, according to UCSD’s Smith.
It’s also likely that outbreaks will continue in places where vaccination rates are low. Infectious disease models rely on population averages, which don’t tell the whole story. If 85 percent of people have been vaccinated, it’s unlikely the remaining 15 percent are spread evenly throughout a community. Some places will have high vaccination rates, and others won’t, either because of differences in access to shots or interest in getting them.
That’s already true in San Diego County, with vaccination rates lower in East County than elsewhere in the region. It’s also true worldwide, with plenty of countries that have only vaccinated a small percentage of their citizens, allowing the virus to spread largely unchecked in places like India.
An uneven vaccine rollout could eventually make coronavirus outbreaks look a bit like measles outbreaks, according to Smith. A single person carrying the measles virus can infect 12 or more people, but the spread of the virus is mostly contained through high vaccination rates. There are, however, still outbreaks in communities where immunization rates are low, such as in Marin County, New York City’s Orthodox Jewish Community and the Philippines. Occasionally, those outbreaks spill out into the wider community.
Smith and Martin say it’s unlikely we’ll ever eradicate the coronavirus — not any time soon, anyway. There’s only one virus scientists have wiped out with a vaccine: smallpox. The World Health Organization began that effort in 1959, declaring the disease eradicated by 1980.
Here’s the good news: Eradication isn’t necessary. The key is vaccinating more people as we return to normal. So far, scientists have yet to find a viral variant that no vaccine works against. Maintaining a high percentage of vaccinated people, which limits the virus’s chances to mutate, will help make sure things stay that way.
“We don’t need to have the goal of eradication to be able to get back to a point as a society where we can live alongside that virus and go about our daily lives with minimal interruption,” Martin said. “You just want to be able to live alongside it so that it doesn’t result in severe disease.”
U-T staff writer Paul Sisson contributed reporting.
[ad_2]
Source link


















