Amazon.com : Medela Pump in Style Advanced with On the Go Tote, Double Electric Breast Pump, Nursing Breastfeeding Supplement, Portable Battery Pack, Sleek Microfiber Tote Bag included with Breastpump : Electric Breast

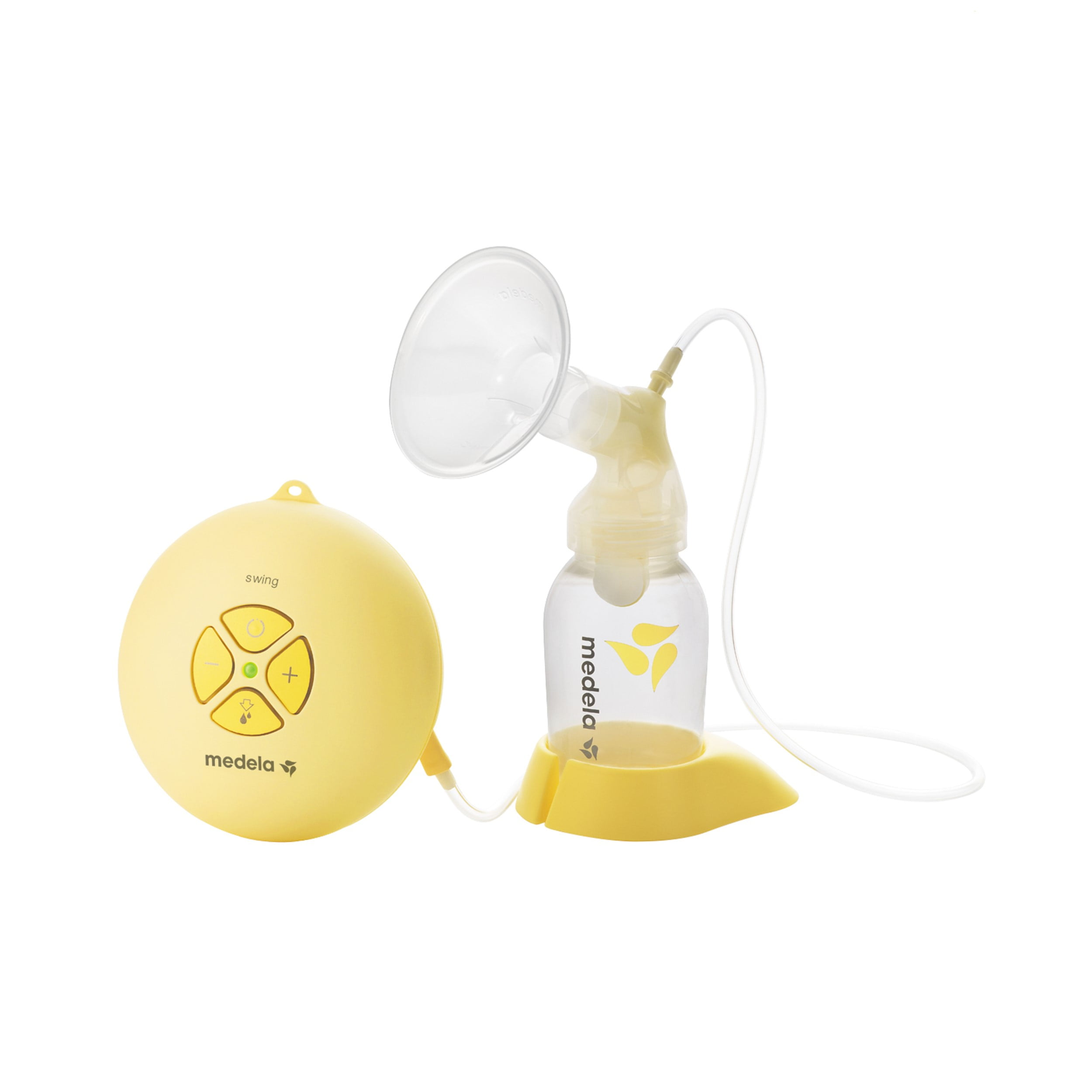
Amazon.com : Medela, Swing, Single Electric Breast Pump, Compact and Lightweight Motor, 2-Phase Expression Technology, Convenient AC Adaptor or Battery Power, Single Pumping Kit, Easy to Use Vacuum Control : Breast Feeding