
Amazon.com: Hot Sweat - Faja de neopreno para sauna, para adelgazar, para pérdida de peso, para mujeres y hombres con cremallera, Negro - : Ropa, Zapatos y Joyería
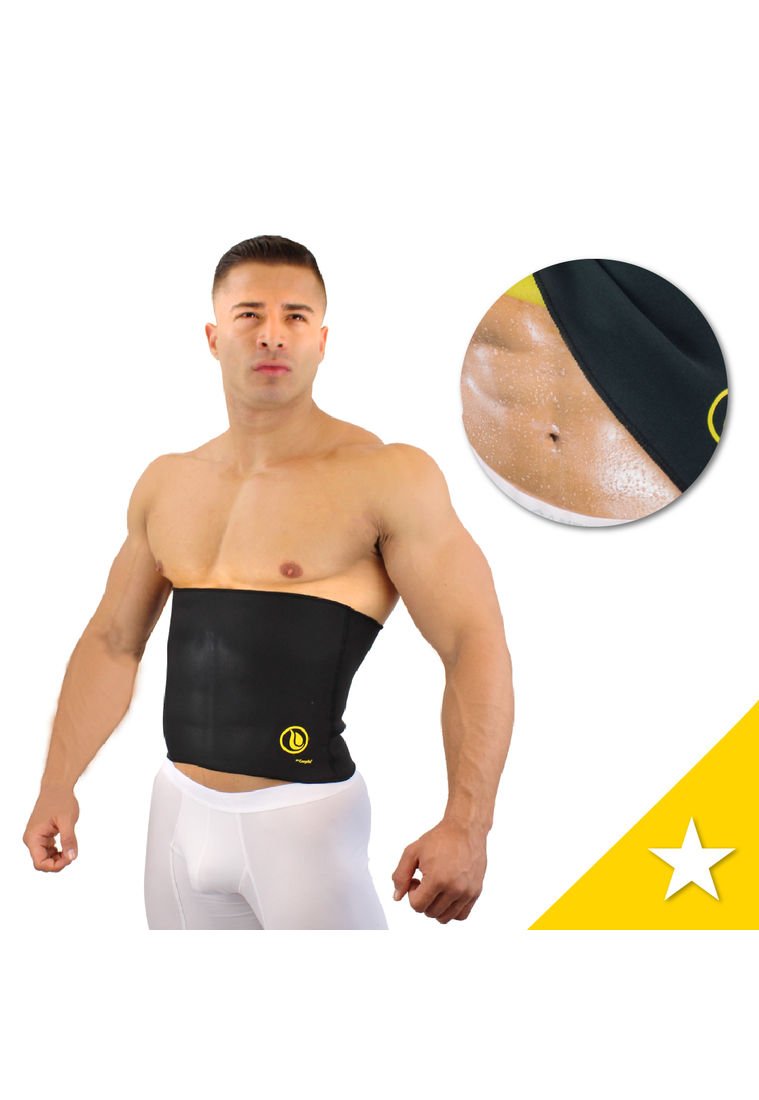
Faja Cinturilla Reductor De Abdomen Para Hacer Ejercicio Y Reducir Cintura Fajas Para Hombre - Compra Ahora | Dafiti Colombia

Amazon.com: MOLUTAN Entrenador de cintura para hombre, para pérdida de peso, control de abdomen, faja de compresión, moldeador de cuerpo, cinturón de sudor, color negro : Deportes y Actividades al Aire Libre

Faja Reductora Modeladora De Abdomen Y Cintura para Entrenamientos, Faja Colombiana Moldea Reduce Abdomen Cintura, Fajas Compresión para Mujer, Fajas Colombiana Que Estiliza Abdomen, Beige, Talla XL : Amazon.com.mx: Ropa, Zapatos y

















:format(jpg)/f.elconfidencial.com%2Foriginal%2Fadf%2Fc60%2Fd86%2Fadfc60d86617aa549dea8ad0decf6d29.jpg)




